
What are shoulder dislocations and why do they reoccur?
The glenohumeral joint (shoulder joint) is a ball and socket joint located between the scapula (shoulder blade) and the humerus (upper arm bone). Structurally, the humeral head fits in the rounded socket of the scapula (the glenoid) and is supported by various ligaments, cartilage, and connective tissues.
Since the shoulder is one of the most mobile joints, with the arm moving in nearly any direction within certain limits, it is incredibly prone to injury. One of the most common reasons for shoulder instability is dislocation, an injury that occurs when the humeral head pops out of the glenoid cavity.

While the humeral head can be put back into place, the underlying damage to the shoulder joint may be more severe. The structures that support the tendons and muscles of the shoulder joint may be stretched or torn during the actual dislocation or may heal improperly in a stretched position.
With damaged tissue, the shoulder loses its stability, which increases the risk of further tissue damage and recurrent shoulder dislocations. [1]
Shoulder Dislocations Recurrence Rates
The shoulder joint has the largest range of motion of any joint in the human body. Unsurprisingly, the shoulder is also the most regularly dislocated joint in the body, accounting for nearly half of all major joint dislocations. [5] It affects an estimated 2 to 8% of the general population.
Following anterior shoulder dislocation, the rate of recurrent instability ranges from 14% to 100%, with patients younger than 20 years old at 72–100%, 20-30 years old at 70–82%, and older than 50 years old at 14–22%. [4]
Similarly, another study found that 87% of patients below 20 years old and 30% of those above 30 will re-dislocate the same shoulder. [6]
How serious is a dislocated shoulder?
A dislocated shoulder is considered a serious and painful injury. While it may seem like the shoulder joint can be “popped back into place” and be healed within a few weeks, shoulder injuries are frequently more complicated than that.
There could be internal damage to nerves, blood vessels, or any structure that reinforces the joint (i.e., muscles, ligaments, tendons). Furthermore, this damage will massively increase the likelihood of future shoulder injuries.
Individuals who suspect a dislocated shoulder should seek medical attention immediately. [2]
Diagnosis and Treatment of Chronic Shoulder Dislocations
As with a first-time shoulder dislocation, your doctor will go through patient medical history, assess potential causes, and conduct a physical examination. Typically, they will want a detailed account of your symptoms and ask about any factors that could increase the risk of another shoulder dislocation.
During the physical exam, the doctor will inspect the shoulder joint area for visible deformities, tenderness, swelling, and areas of pain. While imaging tests are not always necessary for a diagnosis, X-Rays are useful to confirm the diagnosis and reveal any additional damage to internal structures of the shoulder joint.
The treatment for recurrent shoulder dislocations will depend on the severity of the injury. If the patient has a simple dislocation with minimal internal damage, then a doctor might recommend a less invasive treatment plan. This could include:
- Repositioning the humeral head back in the socket.
- An orthotic device, like a splint or sling, to immobilize the arm and shoulder in the correct position, allowing the structures that support the joint to heal.
- Over-the-counter medication to reduce pain and inflammation.
- Rehabilitative exercises. After the initial healing period, you may slowly begin to perform exercises designed to restore flexibility, strength, and stability. [2]
If the imaging tests reveal more substantial damage to any of the structures of the shoulder joint, you may also require surgical treatment. Especially if your shoulder joint and ligaments have been weakened from previous dislocations, surgery can help to tighten or repair the stretched tendons or ligaments.
Can I pop my dislocated shoulder back into place?
Patients should never attempt to reposition the shoulder joint themselves. While it may be tempting to quickly “fix” the dislocation and ease the immediate pain, this may cause more significant damage to any of the surrounding muscles, ligaments, or nerves.
Instead, seek medical attention immediately. As you wait for the doctor, keep the joint immobilized in its current position, and if pain allows, apply ice to the shoulder to minimize pain, swelling, and internal bleeding. [2]
How long should I wear a sling after dislocating my shoulder?
Patients should wear the sling for as long as the doctor has prescribed. In general, this period ranges from two to eight weeks, depending on the nature of the shoulder dislocation.
The purpose of the sling is to limit movement of the arm and shoulder, to allow the joint enough time to heal. It is important not to rush the recovery process, as restarting activity too soon could cause more damage to the joint and its supporting structures.
Rehabilitation can begin after a few weeks of the injury, but only if cleared by the physician or orthopedic specialist.
Prevention and Recovery
To prevent recurrent shoulder dislocation, it is important that you pay careful attention to your shoulder joint and limit activities that increase the risk of dislocation. This includes resting and icing, if pain or soreness reoccurs; wearing extra protective gear when participating in contact sports; and taking extra precautions to avoid falls.
Additionally, patients should incorporate preventative exercises to improve the strength, mobility, and stability of the shoulder joint.
There are several exercises that are specifically designed to strengthen and improve range of motion of the shoulders. They should be performed slowly and deliberately.
- Shoulder flexion. Lying on your back, lift your hands above your head and slowly lower them behind your head until you feel a stretch in your shoulders.
- Shoulder blade squeeze. Standing with your arms by your sides, squeeze your shoulder blades together.
- Internal rotator exercise. Tie a Thera-Band tied to a doorknob. Stand perpendicularly to the band, with your elbow bent at 90º, pull the end of the band inwards towards the stomach.
- Wall push-ups. Stand 1 to 2 feet from a wall and place your hands on the wall, shoulder-distance apart. Lean forward until your chest touches the wall, then push back until your arms are straight again. [7]
Taping to Stabilize the Shoulder Joint
One of the ways to prevent recurrent shoulder dislocations, especially if your joint is already weakened or loose from a prior dislocation, is with some type of bracing. A lightweight shoulder wrap or brace is a good option and is relatively inexpensive.
However, this brace might interfere with the patient’s ability to perform physical activity, so some prefer to use tape. One of the easiest taping procedures to stabilize the shoulder joint after an anterior shoulder dislocation, post-reduction, is with Kinesiology tape. [8]
This type of tape is widely used by physiotherapists to help patients support previously injured areas and prevent further injuries. It works by pulling at the skin gently to stimulate blood flow and reduce swelling.

- Sitting in a neutral position, place one end of a strip of tape at the top of the shoulder. Then using “paper off tension” (about 25% tension), gently guide the tape along the deltoid and down the arm with the leading hand, pulling the backing off as you go. Smooth over the tape with the second hand.
- Applya second piece of tape to the backside, along the posterior deltoid. In a neutral position, place the first end of the tape on top of the shoulder. Then, with the arm stretched across to the body, to the other shoulder, continue to lay the tape with 25% stretch along the arm. Aligning the end of the tape with the first piece.
- Position the affected arm across the chest as far as it can comfortably go and use the other arm to support it in an elevated position. Anchor one end of another piece of tape behind the posterior deltoid. The patient should now roll forward inward to elongate the back. Stretch the tape to 50% stretch and lay it down across the back.
- Anchor the end of a fourth piece of tape just below the piece that was just placed. Stretch it to about 50% tension and lay it along the lower trapezius.
- With a fifth piece of tape, crease it at the center and remove the backing, starting from the middle and moving outwards. With each hand approximately 3 inches from each end of the strip, stretch the tape and place it below the acromion. Bring the arm out to the side and smooth the front 3-inch end of the tape down. Then, with the arm forwards across the chest, smooth the other 3-inch end of the tape. If possible, aim to position this end piece in between the two pieces of tape on the back.
To use this tape effectively, there are a few tips that will facilitate its application:
- Crease the tape 2 inches from the strip’s end to easily remove the backing.
- Do not stretch the tape on the 2-inches at either end of the strip.
- Avoid overlapping the tape whenever possible, as it adheres best to the skin.
- Once applied, smooth over the tape and rub it to activate the adhesive.
- Apply the tape at least 1 hour before normal physical activity and 2 hours before water activity. [8]
Risk Factors for Recurrent Shoulder Dislocations
The largest risk factor for recurrent shoulder dislocation is a previous dislocation or injury, as this leads to shoulder instability. With every shoulder dislocation, the ligaments in the shoulder joint become more stretched or torn and your bones are more likely to move around in the socket. Consequently, the risk factors for shoulder dislocations are also pertain to recurrent dislocations.
- Contact sports. A large number of shoulder injuries occur during high-contact sports. When athletes suffer a hard fall or receive a sudden blow to the shoulder, the blunt force from the contact is sometimes enough to knock the humerus bone out of the socket. Certain contact sports are especially known for causing repeated shoulder dislocations, including football, rugby, and skiing. [2]
- Repetitive overhead activity. Individuals who participate in activities or professions that involve repetitive overhead movements (i.e., lifting objects, cleaning, and painting) or athletes who play overhead sports (i.e., swimming, tennis, and baseball) can overwork the shoulder’s muscles and ligaments. Over time, these structures may weaken or stretch, leading to shoulder instability and dislocations. [3]
- Age. While age itself is not a risk factor, younger individuals are more likely to participate in competitive sports and activities with repetitive overhead movements. More specifically, men under the age of 20 are at the highest risk of dislocating the shoulder joint. [4]
- Genetics. Existing health conditions can also contribute to the risk of shoulder dislocation and reinjury. Some individuals naturally have ligamentous laxity throughout the body, which means that their ligaments are looser and cannot provide the same level of joint support as most people. Consequently, their joints are less stable and are more susceptible to dislocation and other injuries. [3]
What is the difference between shoulder dislocation and shoulder subluxation?
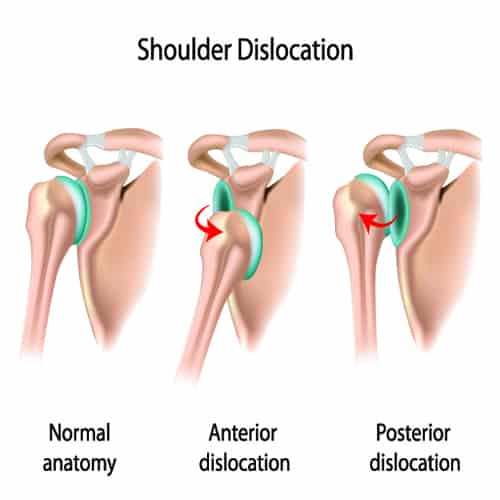
A shoulder dislocation occurs when the humeral head slides completely out of the glenoid cavity, whereas a shoulder subluxation describes a partial dislocation.
With subluxation, the humerus only partially comes out of the socket and the bones that form the joint are still partly connected. [1]
Both injuries are accompanied by pain, swelling, visible deformation, and limited range of motion.
References:
- “Shoulder Instability.” Johns Hopkins Medicine, www.hopkinsmedicine.org/health/conditions-and-diseases/shoulder-instability.
- Mayo Clinic Staff. “Dislocated Shoulder.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 1 Aug. 2020, www.mayoclinic.org/diseases-conditions/dislocated-shoulder/symptoms-causes/syc-20371715.
- Haddad, Amy. “3 Risk Factors for Shoulder Dislocations.” Sports-Health, 21 Nov. 2016, www.sports-health.com/blog/3-risk-factors-shoulder-dislocations.
- Polyzois, Ioannis, et al. “Traumatic First Time Shoulder Dislocation: Surgery vs Non-Operative Treatment.” The Archives of Bone and Joint Surgery, 12 Sept. 2015, www.ncbi.nlm.nih.gov/pmc/articles/PMC4852033/#R13.
- Abrams, Rachel, and Halleh Akbarnia. “Shoulder Dislocations Overview.” U.S. National Library of Medicine, StatPearls Publishing, 1 Nov. 2020, www.ncbi.nlm.nih.gov/books/NBK459125/.
- Robinson, Michael C, et al. “Functional Outcome and Risk of Recurrent Instability after Primary Traumatic Anterior Shoulder Dislocation in Young Patients.” The Journal of Bone and Joint Surgery. American Volume, U.S. National Library of Medicine, Nov. 2006, pubmed.ncbi.nlm.nih.gov/17079387/.
- Burgess, Patrice, et al. “Shoulder Dislocation: Rehab Exercises.” Alberta, 2 Mar. 2020, www.iskinstitute.com/kc/shoulder/shoulder_dislocation/t1.html.
- “KT Tape: Shoulder Dislocation Taping.” YouTube, uploaded by KT Tape, 24 Oct. 2017, www.youtube.com/watch?v=RZ0Y1y0rFOQ.
Elizabeth Miclau is an undergraduate at Harvard College, planning to pursue a concentration in life sciences or sociology. As a member of both Puerto Rico’s National Diving Team and Harvard’s Women’s Varsity Swimming and Diving Team, she has a strong background in elite athletics. In the past year, she has contributed to several journal publications and peer-review-funded research projects.