The Achilles tendon (tendo calcaneus or tendo Achillis) is the band of fibrous tissue running along the back of the lower leg and foot, connecting the calf muscles to the heel bone.
More specifically, the gastrocnemius and soleus (calf) muscles join together near the base of the leg to merge with the Achilles tendon, which then inserts into the calcaneus (heel bone).
There are two bursae in the foot, which are fluid-filled sacs that cushion these tendons and bones. The subcutaneous calcaneal bursa helps the skin glide easily over the tendon and the retrocalcaneal bursa reduces friction between the Achilles tendon and heel bone. [1]

The Achilles tendon is the thickest and strongest of the human body. [2] On average, the Achilles tendon is 15 centimeters long, but it can range anywhere from 11 to 26 cm.
It is thickest near the calf muscles, with a mean width of 6.8 cm, and gradually narrows to 1.8 cm near the upper heel. At its insertion into the calcaneus, the tendon becomes rounded and slightly thicker at 4 cm. Recent research reports that the calcaneal insertion’s crescent shape plays an important role in distributing stress from the tendon onto the calcaneus. [3]
Blood is supplied to the lower leg by three main arteries: the peroneal artery, the anterior tibial artery, and the posterior tibial artery. The Achilles tendon receives the majority of its blood supply at its proximal and distal sections from the posterior tibial artery.
Due to poor vascularity near the middle of the tendon, the peroneal artery only contributes minimal amounts of blood. The anterior tibial artery is not known to supply blood to the tendon. [3]
Overall, the Achilles tendon has a limited blood supply, with a relatively low number of vessels per cross-sectional area. In most cases, blood flow to the Achilles tendon further diminishes with age. [2]
What does the Achilles tendon do?
The Achilles tendon is responsible for plantar flexion in the foot – the motion of pointing the toes down, away from the leg. In response to the contraction of the calf muscles, the Achilles tendon pulls on the heel to raise it off the ground.
The tendon also absorbs shock forces on the foot and can withstand tensile loads of up to ten times the body’s weight. [3]
Consequently, the Achilles tendon is implicated in any activity requiring an extension of the ankle, such as walking, running, and jumping.
Why is it called “Achilles heel”?
The term “Achilles heel” originates from the myth of Achilles, the hero of the Trojan war. According to Greek mythology, Achilles was held by the ankle and dipped him in the river Styx by his mother, Thetis, in an attempt to make him immortal.
Despite being the strongest warrior of the Trojan war, he was killed after taking a poisoned arrow to his only point of vulnerability– the heel that was not dipped in water.
Today, the proverbial “Achilles heel” designates a point of weakness and vulnerability. [3]
Common injuries
While the Achilles tendon is the thickest and strongest of the human body, its combination of heavy tensile load and poor blood supply make it particularly vulnerable to injury.
Achilles tendon injuries usually come as a result of overuse or overload and can be very painful.
- Achilles tendon ruptures are a partial or complete tear in the tendon’s fibers, causing severely impaired movement in the foot. Achilles tendon ruptures only occur in 5 to 10 cases per 100,000 in North America, with the majority happening during high-level sporting activity. [2] Rupture of the Achilles tendon may make a “pop” sound.
- Achilles Tendinopathy is the most common cause of tendon pain near the heel, which accounts for nearly 60% of cases. [2] Achilles tendinopathy is a general term that encompasses both Achilles tendinitis and tendinosis.
- Achilles Tendinitis refers to the inflammation of the tendon, which can either be non-insertional and insertional. Non-insertional Achilles tendinitis is characterized by small tears in the tendon’s fibers, whereas insertional tendinitis describes fiber degeneration where the tendon inserts into the heel bone. [4]
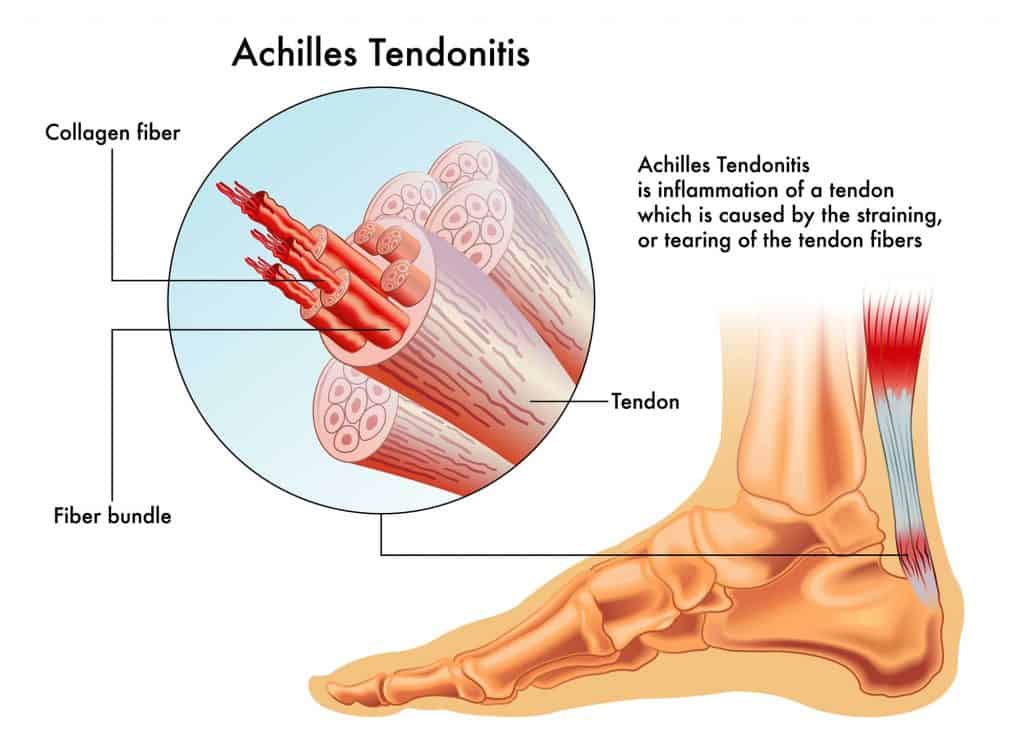
- By comparison, tendinosis designates the gradual thickening of the tendon which causes it to weaken. [2]
- Achilles bursitis happens when the retrocalcaneal bursa becomes irritated. The retrocalcaneal bursa is a fluid-filled sac that acts as a cushion between the Achilles tendon and the calcaneus. [1]
How do I know if I have Achilles tendinitis or tendinosis?
The terms “Achilles tendinitis” and “Achilles tendinosis” are frequently confused with one another, but they represent two distinct conditions.
Tendinitis describes the acute inflammation or microtears in the Achilles tendon which result from a sudden overload or overuse. By contrast, tendinosis is a chronic condition characterized by the degradation of the tissue fibers in the Achilles tendon.
Achilles tendonitis can usually resolve itself with weeks of conservative treatment, whereas tendinosis may require more specialized medical treatment.
Individuals who experience Achilles tendon pain should consult with a physician for a proper diagnosis. [5]
Are some Achilles tendon injuries more serious than others?
Yes, certain Achilles tendon conditions may be considered more serious than others.
For example, microtears in the fibers of the Achilles tendon may only need temporary conservative measures to be resolved, whereas a complete rupture of the tendon will likely require more aggressive treatment.
However, any damage to the Achilles tendon should be taken seriously and treated appropriately.
When should I see the doctor for Achilles tendon pain?
Following an overuse or overload on the Achilles tendon, individuals may experience mild pain or discomfort near the heel.
This injury may not require medical attention and should be treated with conservative measures.
In the case that symptoms persist or begin to interfere with everyday functional activity, then it is highly advisable to contact a physician.
Medical Diagnosis
It is often difficult to determine the cause of Achilles tendon pain without a proper medical diagnosis. Most physicians will only need to conduct a physical examination of the foot to determine the nature of the injury.
However, many diagnostic tests may be used to confirm the suspected diagnosis or to rule out other injuries.
In a physical examination, patients can expect the physician to check their foot and lower leg for any bone growth, swelling, and discoloration around the tendon. They will also move the ankle around to evaluate its range of motion, reflexes, and stiffness.
They may conduct tendon reflex tests, namely the Thompson and Matles tests. For the Thompson test, the patient lies face-down, and the physician squeezes the calf to contract the muscles.
If the heel does not pull up in response, it may be an indication that the Achilles tendon is ruptured. Similarly, during the Matles test, the patient lies face-down and will slowly bend their knee to a perpendicular position. If the top of their foot does not slightly angle away from the leg, then the Achilles tendon may be ruptured. [1]
If the findings from the physical exam are not enough for a diagnosis, the physician may also order one of the following diagnostic tests:
- MRI scan. Magnetic resonance imaging scans generate detailed images of bones, joints, and soft tissues, and can detect an Achilles tendon rupture.
- Ultrasound. Ultrasounds create detailed images of the soft tissues in the body and can also detect an Achilles tendon rupture.
- CT scan. Computed tomography scans combine multiple X-rays to create detailed cross-sectional images of internal organs, bones, and soft tissues. CT scans may help to better visualize the lower leg and ankle.
- X-ray imaging. X-rays also produce detailed images of structures within the body and can be especially helpful to examine the bones in the lower leg.
Treatment and Recovery
Most Achilles tendon conditions can be resolved within a few months with conservative treatment. This usually involves a combination of the RICE method, pain relievers, orthotic immobilization devices, and physical therapy.
The RICE method – Rest, Ice, Compression, and Elevation – is a simple at-home treatment that helps accelerate the recovery process.
- Rest prevents further damage by eliminating strain on the tendon;
- Ice reduces swelling and relieves pain near the tendon;
- Compression stabilizes the tendon and restricts blood flow to reduce swelling; and
- Elevation will also reduce swelling, pain, and discomfort. Nonsteroidal pain medication may be taken in conjunction with these measures to further alleviate pain and inflammation. [6]
Depending on the damage to the Achilles tendon, immobilization may be necessary for recovery. Mild inflammation of the tendon will not usually require more than a brace to compress and stabilize the tendon.
However, more severe Achilles tendon injuries may involve complete immobilization with a boot or cast. Patients should refer to their physician to determine if an orthotic immobilization device is needed.
Surgery is usually only required to repair a severely torn or ruptured Achilles tendon.
References:
- Hoffman, Matthew. “Achilles Tendon (Human Anatomy): Picture, Definition, Injuries, Pain, and More.” Jumpstart by WebMD, WebMD, 18 May 2019, www.webmd.com/fitness-exercise/picture-of-the-achilles-tendon#1.
- Physiopedia contributors. “Achilles Tendon.” Physiopedia, 1 Oct. 2020, www.physio-pedia.com/Achilles_Tendon.
- Doral, Mahmut Nedim, et al. “Functional Anatomy of the Achilles Tendon.” Knee Surgery, Sports Traumatology, Arthroscopy, SpringerLink, 25 Feb. 2010, link.springer.com/article/10.1007/s00167-010-1083-7.
- “Achilles Tendinopathy – Orthopaedic Injuries of the Foot.” Dr. Alex Meininger Orthopaedics and Sports Medicine, 30 June 2020, www.dralexmeininger.com/injuries-conditions/achilles-tendinitis/.
- Cafasso, Jacquelyn. “Tendonosis: Symptoms, Treatment, and Recovery Time.” Edited by William Morrison, Healthline, 19 July 2017, www.healthline.com/health/tendonosis.
- Ambardekar, Nayana. “RICE Method for Injuries (Rest, Ice, Compression, Elevation).” WebMD, 30 Apr. 2019, www.webmd.com/first-aid/rice-method-injuries.
Elizabeth Miclau is an undergraduate at Harvard College, planning to pursue a concentration in life sciences or sociology. As a member of both Puerto Rico’s National Diving Team and Harvard’s Women’s Varsity Swimming and Diving Team, she has a strong background in elite athletics. In the past year, she has contributed to several journal publications and peer-review-funded research projects.