What is Achilles Tendinitis?
Achilles tendinitis occurs as a result of overuse or damage to the Achilles tendon, which causes pain on the back of the leg near the heel. [1]
The Achilles tendon (tendo calcaneus or tendo Achillis) is the band of fibrous tissue that connects the calf muscles to the heel bone, allowing you to raise and lower your heels. Normally, when the calf muscles are flexed, the Achilles tendon pulls on the heel and raises it off the ground.
However, when high tensions are placed on the tendon, this movement may become restricted and painful.
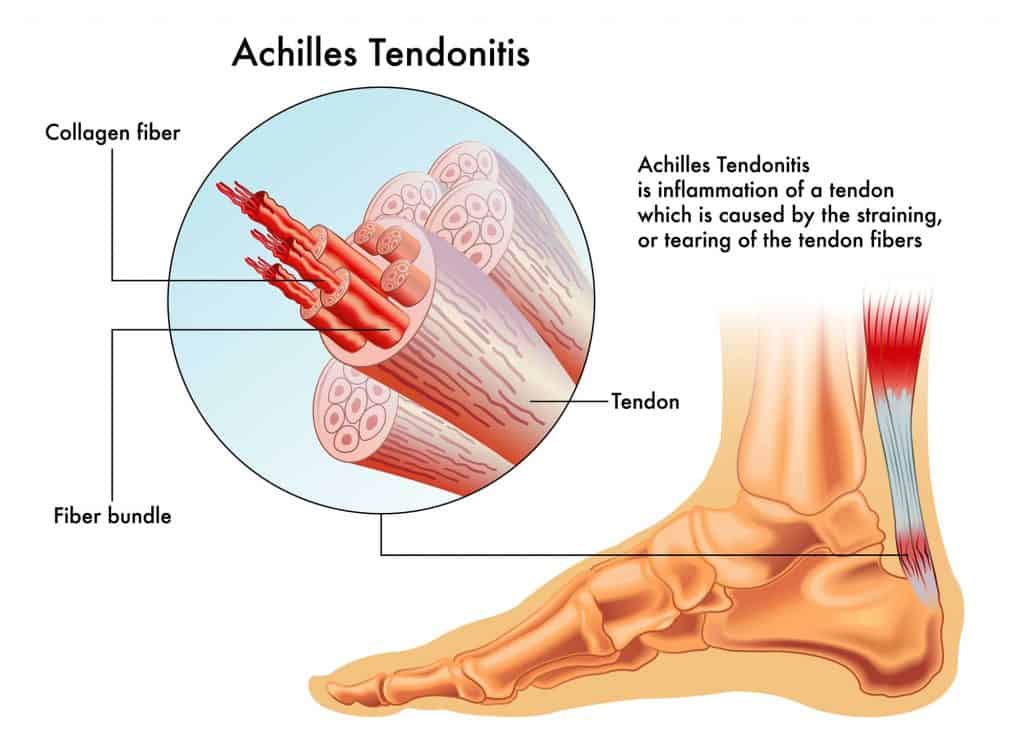
There are two types of tendonitis: non-insertional and insertional. Non-insertional Achilles tendinitis is characterized by small tears in the fibers of your tendon and typically affects younger active individuals, whereas insertional Achilles tendinitis describes damage to the area when the tendon and heel bone connect, and generally affects people of all ages.
Who is most affected by Achilles tendinitis?
The majority of people affected by Achilles tendinitis are runners and athletes engaged in high-intensity activity. The excessive pronation and load-induced stress of running and jumping strains the Achilles tendon, causing inflammation and pain. [2]
However, it is also common for middle-aged individuals to develop Achilles tendinitis after prolonged periods of walking, running, or other physical activities. [1]
Symptoms
Achilles tendinitis usually begins with mild pain near the lower calf and upper heel after strenuous physical activity.
Often, the pain is accompanied by inflammation, tenderness, or stiffness, and will worsen with activity. You may have difficulty walking, pointing your toes, or raising your heels off the ground.
How do you know if your Achilles tendon is torn or ruptured?
When the Achilles tendon is subject to strenuous physical activity, it can become inflamed or irritated, which causes pain, swelling, and stiffness in the area between the calf and heel.
However, an obvious indication that your Achilles tendon has torn or ruptured is if you hear a loud snapping or popping noise in the back of your leg, followed by immediate and severe pain.
If you suspect that you’ve torn your Achilles tendon, you should seek medical attention immediately as your injury may require surgical treatment. [3]
How can you tell the difference between Achilles tendonitis and plantar fasciitis?
While Achilles tendonitis and plantar fasciitis are both characterized by pain and inflammation near the heel, there are many differences between the two.
Plantar fasciitis is an inflammation of the plantar fascia, the fibrous ligament that connects the toes to the heel bone, and is characterized by pain on the bottom of the foot near the heel.
Typically, pain is most severe in the morning, but should improve with some walking or stretching.
By contrast, Achilles tendinitis is characterized by the inflammation of the Achilles tendon, the fibrous band of tissue connecting the calf muscles to the heel bone. This strain on the tendon causes pain in the lower calf and upper heel, and will usually worsen with more activity. [4]
Causes and Risk Factors
Achilles tendinitis is caused by an overuse or overstrain of the Achilles tendon, which can be intensified by a number of factors, including:
- Age: Similar to other tendons and connective tissues in the body, the structure of the Achilles tendon weakens with age. With a decreased strength and stiffness, the tendon is more vulnerable to damage and injury. Consequently, Achilles tendinitis is most prevalent in individuals between the ages of 30 and 50. [5]
- Gender: Achilles tendon injuries are nearly five times more likely to occur in men, which may be linked to sex-differences in the physical properties of the Achilles tendon. [6]
- Foot mechanics: The structure and natural pronation of the foot may be adding additional strain on the Achilles tendon.
- Footwear: Wearing worn-out or shoes with inadequate arch support may increase the risk of developing Achilles tendonitis. Certain shoes may prevent the Achilles tendon from reaching a fully extended position, which could limit its normal range of motion. [1]
- Medical conditions: Individuals with medical conditions, such as high blood pressure or obesity, are more vulnerable to developing this condition, as blood flow to the Achilles tendon may be diminished. [5]
- Medications: Certain antibiotics have been closely linked with elevated rates of Achilles tendinitis. [1]
Can walking barefoot cause Achilles tendinitis?
While walking barefoot on hard surfaces will not likely be the sole cause of Achilles tendonitis, it is inadvisable as your foot will not have extra cushioning or support.
The structure of your foot governs how pressure and weight is distributed throughout the foot. Without the arch support of shoes or slippers, your feet may collapse and put unnecessary strain on ligaments, tendons, and muscles.
It is also important to note that excessive walking, either barefoot or with shoes, may cause Achilles tendinitis.
Diagnosis
Achilles tendinitis is diagnosed based on patient medical history, an assessment of risk factors, a physical examination, and imaging tests.
Typically, your doctor will ask for a detailed description of your symptoms and inquire about any factors that could increase the risk of developing this condition.
Next, your doctor will conduct a physical examination to check your Achilles tendon for bone growths, pain, or swelling. They will also move your foot and ankle around to evaluate its flexibility, range of motion, and reflexes.
Sometimes, they may also order imaging tests to assess the severity of your condition and determine the best course of treatment. X-rays can detect bone spurs or calcified tendons, ultrasounds visualize soft tissues and blood flow around the tendon, and MRIs provide a clear image of the Achilles tendon. [1]
Treatment and Recovery for Achilles Tendinitis
In the majority of cases, Achilles tendinitis can be resolved within a few months with conservative treatment. Simple strategies include the RICE treatment, anti-inflammatory medication, stretching exercises, and orthotic devices.
The RICE method –Rest, Ice, Compression, and Elevation– is one of the most frequently recommended treatments for soft tissue injuries.
- Rest will prevent further strain on the Achilles tendon and give the body time to recover;
- Ice will reduce swelling, stimulate blood flow, and relieve pain near the tendon;
- Compression will stabilize the tendon and reduce swelling;
- Elevation will also reduce swelling, pain, and discomfort. [1] Similarly, over-the-counter pain medication will alleviate many of the symptoms.
Physical therapy is also widely recommended as it will help patients stretch the Achilles tendon and strengthen the calf muscles.
More specifically, individuals with Achilles tendon injuries have had significant success with “Eccentric exercises”. This specific type of strengthening consists of heel-lowering movements which are designed to lengthen your muscles under tension.
In the case that your symptoms do not improve after six weeks, your doctor may suggest a number of other treatments. This could include extracorporeal shockwave therapy, blood or platelet-rich plasma (PRP) injections, low-level laser therapy, or dry needling. [7]
If symptoms continue to persist after many months of treatment or if the tendon tears, your doctors may recommend surgery to repair your Achilles tendon. [1]
Will compression socks or an ankle wrap help with Achilles tendonitis?
Orthotic devices, like compression socks or ankle wraps, provide additional cushioning that may relieve some of the strains and forces on your Achilles tendon. [2]
The compression increases blood flow around the tendon and will promote more circulation of oxygen and nutrients.
However, compression alone will not be enough to cure this condition –compression should be coupled with rest, icing, and elevation, as well as physical therapy exercises, proper footwear, and other conservative measures.
How much rest do you need for Achilles tendonitis?
The amount of time needed to rest the tendon will depend on the severity of your condition.
It is recommended that you avoid the activity that triggered your symptoms and rest until your pain begins to improve.
Then, you may begin doing some easy stretches and gradually shifting weight onto your affected leg. It is important not to rush recovery as this may further damage your tendon.
Should I see a doctor for Achilles tendon pain?
Yes. If you are experiencing pain, swelling, tightness, or a limited range of motion in the heel and foot, it is important to see a doctor.
Achilles tendon pain may be an indication of Achilles tendinitis, which would make your tendon more susceptible to tears and ruptures.
A torn or ruptured tendon is a serious injury that often requires surgery to repair. [2]
Should you stretch a strained Achilles?
Ideally, you would not stretch a strained Achilles. It is best to avoid adding any additional strain on your tendon, as an inflamed tendon is particularly vulnerable to tears and ruptures.
Instead, you should rest your leg until your pain starts to subside. Then once the pain has improved, you may begin with slow and gentle stretches. [5]
What exercises are recommended, and what exercises should be avoided during rehabilitation for Achilles tendonitis?
The American Academy of Orthopaedic Surgeons (AAOS) and the National Health Service (NHS) recommend specific “Eccentric” exercises that can improve range of motion of the foot and reduce the stress on the tendon.
Stretching the tendon and strengthening the surrounding structures will decrease the risk of further injury. Common exercises include heel raises on the ground, heel raises off of a ledge, standing gastroc and soleus stretches, slow step-ups, and towel stretches.
Any exercise with sudden movements, like running or bouncing, may further aggravate the tendon and should be avoided. [3]
Will heat help improve Achilles tendonitis?
A combination of ice and heat may help to relieve Achilles tendonitis pain and reduce inflammation.
For the first few days following a tendon injury, it is highly recommended that you follow the RICE treatment method – Rest, Ice, Compression, and Elevation.
Icing for 15-20 minutes several times a day will numb the affected area and constrict the blood vessels to reduce swelling and alleviate pain. However, once the inflammation is reduced, heat may be more beneficial for pain management.
The heat increases blood flow to the tendon and relaxes your calf muscles, which should promote healing and pain relief. [8]
Prevention
There are many measures that can be taken to decrease the risk of developing Achilles tendinitis. Among these strategies include:
- Stretching. Stretching your Achilles tendon and calf muscles will help improve flexibility and mobility in the foot and ankle. This will ultimately loosen and reduce stress on the tendon.
- Strength exercises. The Achilles tendon and calf muscles are subject to the stresses of physical activity. By strengthening these muscles, you will reduce strains put on the tendon and reduce the likelihood of injury and pain.
- Gradually increase physical activity. Ease into strenuous activity by incrementally increasing the duration and intensity of your exercise. This will ensure the tendon and calf muscles are adequately flexible and strong to handle the pressures on the leg and foot.
- Footwear. It is important to wear shoes with sufficient arch support and cushioning to distribute shock forces evenly throughout the foot and reduce unnecessary strain on the tendon.
- Modifying strenuous activity. Limit high-impact activities, like jumping or running, if they cause any discomfort or pain. Instead, consider incorporating other lower-impact activities to allow your tendon time to recover and regain strength. [1]
References:
- Mayo Clinic Staff. “Achilles Tendinitis.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 17 Sept. 2019, www.mayoclinic.org/diseases-conditions/achilles-tendinitis/symptoms-causes/syc-20369020.
- Winters, Brian S. “5 Facts From Surgeons For Achilles Pain Tendonitis.” Rothman Orthopaedic Institute, 5 Oct. 2015, rothmanortho.com/stories/blog/5-facts-from-surgeons-for-achilles-pain-tendonitis.
- Barrell, Amanda. “What Are the Best Stretches for the Achilles Tendon?” Edited by Daniel Bubnis, Medical News Today, MediLexicon International, 20 May 2020, www.medicalnewstoday.com/articles/achilles-tendon-stretches#causes-of-pain.
- “Heel Pain: Achilles Tendonitis vs. Plantar Fasciitis.” Minneapolis Vein Center, 24 Apr. 2016, www.mplsvein.com/blog/heel-pain.
- Carcia, Christopher R et al. “Achilles pain, stiffness, and muscle power deficits: achilles tendinitis.” The Journal of Orthopaedic and Sports Physical Therapy vol. 40,9 (2010): A1-26. doi:10.2519/jospt.2010.0305
- Saltsman, Kirstie. “Sex-Differences in Achilles Tendon Properties May Explain Why Ruptures Occur More Often in Men.” National Institute of Arthritis and Musculoskeletal and Skin Diseases, U.S. Department of Health and Human Services, 20 Dec. 2016, www.niams.nih.gov/newsroom/spotlight-on-research/sex-differences-achilles-tendon.
- McClelland, Damian. “Achilles Tendinopathy.” Bupa UK, www.bupa.co.uk/health-information/muscles-bones-joints/achilles-tendinopathy.
- Laskowski, Edward R. “Tendinitis Pain: Should I Apply Ice or Heat?” Mayo Clinic, Mayo Foundation for Medical Education and Research, 8 Oct. 2020, www.mayoclinic.org/diseases-conditions/tendinitis/expert-answers/tendinitis/faq-20057872.
Elizabeth Miclau is an undergraduate at Harvard College, planning to pursue a concentration in life sciences or sociology. As a member of both Puerto Rico’s National Diving Team and Harvard’s Women’s Varsity Swimming and Diving Team, she has a strong background in elite athletics. In the past year, she has contributed to several journal publications and peer-review-funded research projects.