An injury to the ligament [overstretching or tearing of fibers] is called a sprain. Ligaments are tough fibrous tissues that link two bones in a joint and provide support and limit excessive movements.
The ligaments of the knee are categorized into two: the cruciate ligaments consisting of the ACL (anterior cruciate ligament) and the PCL (posterior cruciate ligament); and the collateral ligaments consisting of the MCL (medial collateral ligament) and the LCL (lateral collateral ligament).

A tear occurs when the body’s soft tissues, such as a muscle, ligament, or cartilage, are ripped apart in two or separated from its bone attachment.
If you are struggling to identify if your knee injury is a sprain or tear, read our blog post.
Types of Knee Sprains
A sprain in any of the ligaments is graded based on the following:
- Grade 1 or Mild
- The ligament stretches, and the only visible damage is microtears. The knee is still stable and can support the body.
- Grade 2 or Moderate
- The ligament partially or incompletely tears. There is some instability in the knee, and the knee might feel like it will give out.
- Grade 3 or Severe
- The ligament tears completely. The knee is unstable, and putting weight on the affected leg is difficult.
Types of Knee Tears
Knee tear occurs when any of the ligaments or menisci are ripped apart or separated from the bone where it attaches. The ligament or meniscus can be partially damaged or fully damaged, or detached from the bone. Knee tears are classified into three types:
Cruciate Ligament Tears
- The ACL is the most commonly torn ligament and occurs mostly as a result of athletic activities. The PCL is the strongest ligament among the four ligaments of the knee; thus, it is less commonly injured.
- ACL tears can be caused by forceful rotation of the knee, sudden stops when running, twisting or changing direction, and landing on a twisted knee after a jump.
- The leading cause of PCL tear is motor vehicle accidents resulting in injury derived from contact with the dashboard. When the PCL tears, there is a high possibility that other structures in the knee are also damaged.
- The ACL and the PCL cross each other to form the “X” structure in the middle of the knee joint. They are responsible for stabilizing the knee and preventing the lower leg’s bone from slipping forward or backward excessively relative to the thigh bone.
Collateral Ligament Tears
- The MCL and the LCL are ligaments at the knee’s inner side and outer side, respectively. The MCL is attached from the inner side of the thigh bone (femur) to the bigger bone of the lower leg (tibia) and prevents the lower leg from moving excessively inward.
- MCL and LCL tears are fairly uncommon to occur independently and are usually accompanied by a tear in either of the cruciate ligaments. Similar to the ACL, collateral ligament tears are frequently obtained through contact sports.
- A strong force or impact is usually responsible for MCL and LCL injuries during contact sports like football. These ligaments can also tear when falling sideways, forcing the knee to bend in an awkward position.
- It is relatively uncommon for the LCL to tear on its own; a tear usually accompanies damage to one or more knee structures.
Meniscal Tears
- The menisci of the knee face each other to form a ring that encircles the ACL and the PCL located in the middle of the knee joint. Meniscal tears are commonly known as “torn cartilage,” and they also occur due to contact sports injury.
- Meniscal tears usually occur during contact sports. Extreme rotation and excessive pressure in the knee typically cause a tear in one of the menisci. Activities such as deep squatting, sudden twisting, and heavy lifting may also damage the meniscus.
- As we age, the meniscus degenerates. Over time, the micro-tears acquired from daily activities may not heal as well as they should, possibly progressing to degenerative tears. Thus, degenerative meniscal tears are common among elderly individuals. When this happens, simple tasks such as rising from a chair can easily injure the meniscus.
Causes of Knee Sprains Tears
A knee sprain can be due to a sudden force or movement that causes stress to the knee’s ligaments.
ACL sprain or tear can happen due to sudden stopping, twisting, pivoting, or changing direction or when there is direct and forceful impact at the back of the lower leg.
The most common cause of PCL sprain or tear directly impacts the front of the lower leg, such as in a “dashboard injury” typical in automobile accidents. It can also occur due to landing hard when the knee is bent during a sports activity.
A blow on the outer side of the knee that moves the lower leg excessively inwards results in an MCL sprain or tear. An impact on the inner side of the knee that moves the lower leg excessively outwards results in an LCL sprain or tear. Injuries to both collateral ligaments can occur due to sports and activities that require frequent twisting or pivoting.
Meniscal tears can occur when there is excessive pressure or extreme rotation on the knee. Activities that may cause a tear in any of the menisci include deep squatting, sudden twisting, and heavy lifting.
A worn meniscus due to age or micro-tears that occurred over time may result in degenerative tears. These are common in elderly individuals, which puts them at risk for damaging the meniscus even with simple activities such as awkward stepping during walking or getting up from a chair.
Damage to a single knee structure is fairly uncommon; most are a combination of different structures as they work together as a unit.
The “unhappy triad” is a severe injury to the knee joint that involves damage to the ACL, MCL, and medial meniscus. When the foot is planted on the ground, the knee is slightly bent, and there is forceful twisting or rotating on the knee.
Treatment
The RICE protocol is frequently recommended by doctors for Grade I or II knee sprain. It stands for:
- Rest the affected leg and avoid weight-bearing
- Ice the injured part for 20 minutes to lessen the pain and swelling.
- Compress using an elastic bandage or sleeve.
- Elevate above the level of the heart.
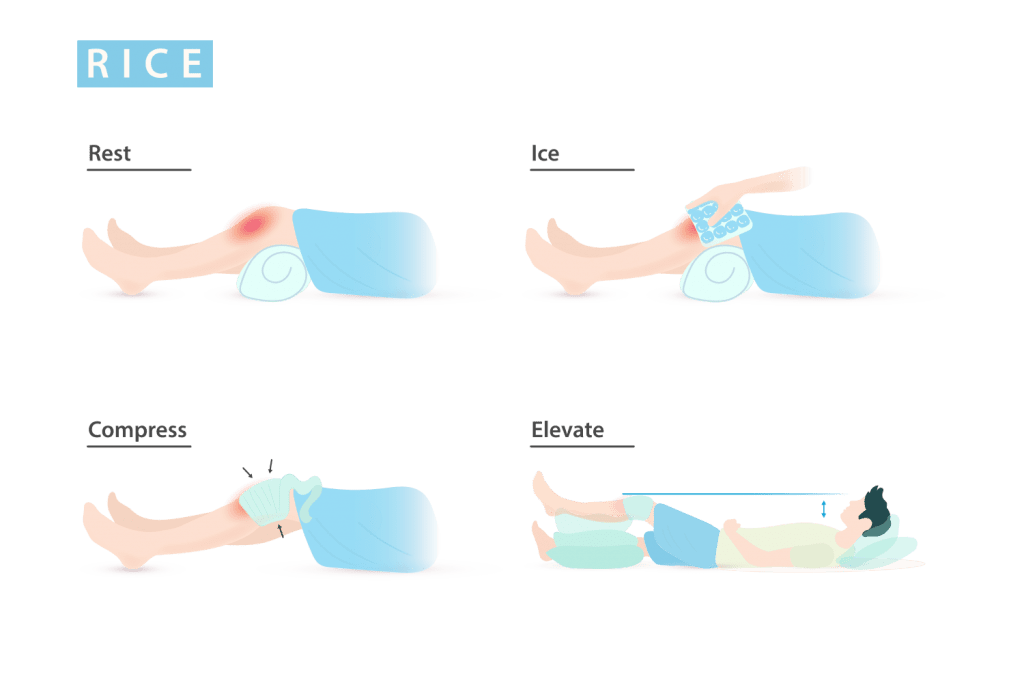
Although the RICE protocol has been used for decades, several studies have debunked it and claimed that it could even hinder tissue healing.
Instead of the RICE protocol, the PEACE and LOVE are being suggested by many orthopedics and physical therapists. Immediately after a soft tissue injury, it is recommended to perform PEACE which stands for:
- Protect the area by restricting movement for 1 to 3 days.
- Elevate higher than the heart.
- Avoid anti-inflammatory modalities such as medication and use of ice which can potentially delay tissue healing.
- Compress using bandage or tape.
- Educate the patient in his/her condition, recovery time, and the importance of active participation.
After a few days of healing, LOVE is suggested, which stands for:
- Load the injured part using active, controlled exercises to promote repair and healing.
- Optimism should be encouraged to lessen the effect of barriers to recovery such as fear and depression.
- Vascularization through early mobilization and aerobic exercise to improve function and facilitate return to activity.
- Exercise to restore mobility, strength, and function while avoiding pain and using it to guide exercise progression.
Knee injuries are mostly managed conservatively. However, severe damage to the knee structures may require surgery depending on which structure is affected, the extent of the injury, and the individual’s lifestyle.
Rehabilitation
Physical therapy intervention is usually enough to manage knee sprain or tear. Whether the doctor recommends conservative treatment or surgery, both will require physical therapy management.
It aims to strengthen the muscles of the knee, restore normal range of motion, improve balance and coordination, and facilitate proper body mechanics and joint conservation techniques.
Physical therapy aims to depend on the type of knee injury, the goal of the patient and referring physician, and the lifestyle, occupation, and daily activities of the patient.
Exercises are usually done in a slow, progressive manner. It includes direct strengthening of muscles, flexibility, balance, and aerobic exercises for general body conditioning.
Questions to Ask Your Doctor
Sustaining an injury and recovering from it is a long and difficult process. Having the proper knowledge could save one from obtaining another injury or causing re-injury to the already vulnerable knee.
These are some of the questions that can be asked during a visit to the doctor:
- What are the activities that I can perform while recovering from the injury?
- How do I prevent re-injury on the same leg or the same injury on the unaffected leg?
- What are the things that I should look for that indicate that my injury is getting worse?
- What should I expect from physical therapy?
- How can I say that I am doing the exercises correctly and not harming the injured leg?

Dr Aarti is an MBBS (Bachelor of Medicine and Surgery) from Baroda Medical College (The Maharaja Sayajirao University, Baroda). Dr. Aarti has also completed her Masters of Medical Science and Technology from the prestigious Indian Institute of Technology, Kharagpur.

